Chapter.03/07
The Technologies Behind Digital Health
- Three Technologies Unite to Remake Digital Health
- Putting It All Together
- Exploring the Genome
- Diagnosing, Predicting and Preventing Disease
- Need Answers? Ask the AI
- AI in Practice
- The Challenge and Potential of Big Data
- Goal: Health Data on 1 Million Americans
- Rise of the (Tiny) Machines
- Small Tech, Big Impact
- Technological Innovation: The Key to Digital Health
The Technologies Behind Digital Health
Chapter 03/07
The Technologies Behind Digital Health
- Three Technologies Unite to Remake Digital Health
- Putting It All Together
- Exploring the Genome
- Diagnosing, Predicting and Preventing Disease
- Need Answers? Ask the AI
- AI in Practice
- The Challenge and Potential of Big Data
- Goal: Health Data on 1 Million Americans
- Rise of the (Tiny) Machines
- Small Tech, Big Impact
- Technological Innovation: The Key to Digital Health
Snapshot
Learn about the remarkable technologies that are making the digital health revolution possible. Explore breakthroughs such as genomics, artificial intelligence, big data, nanotechnology and cloud computing.
Key Terms:
- Human genome
- Genomics
- Wi-Fi
- Sensor
- Cloud computing
- Precision medicine
- Artificial intelligence (AI)
- Big data
- Nanotechnology
Digital health is causing radical changes in the way we prevent, diagnose and treat disease—for the better.
Care providers are beginning to use remarkable improvements in genetic sequencing to target interventions to each person’s genome. Powerful supercomputers are helping physicians make better treatment decisions. Wearable health sensors can detect heart problems instantly. Scientists are creating tools the size of a molecule that can diagnose illness and deliver medications.
What makes it all possible are the remarkably sophisticated technologies powering these innovations. Some of the most advanced technology in the world is being put to use in novel ways to attack disease and save lives.

Three Technologies Unite to Remake Digital Health
The kind of tech most of us are familiar with is usually in our pockets or on our wrists—everyday devices that help us check the weather, monitor traffic, stay in touch with people and make it to appointments on time. And yet that very tech is also pushing digital health into the future by combining three types of technology—wireless devices, sensors and the cloud—into a single device.
Wireless Devices
“Wireless” refers to any technology that transmits data through the air via radio frequencies, infrared or satellite instead of using wires. Technically, cordless phones, TV remote controls and automobile GPS systems are wireless devices. Your cellphone is wireless, whether it’s using a cellular network or a local wireless internet connection (known as Wi-Fi). A host of computer peripherals also operate wirelessly, typically through Bluetooth connections, so you can use a printer, mouse, keyboard or headset with your computer with no wires involved. And computers themselves are wireless any time they connect to a wireless peripheral or use a Wi-Fi signal to connect to the internet.
Sensors
A sensor is an electronic device designed to measure information about its physical environment.
Simply put, a sensor is an electronic device designed to measure information about its physical environment and send that information to another electronic device. The thermostat in your home or your car, the motion-detector light on your front porch, the infrared sensors that make a public toilet flush—these are all examples of sensors at work.
Cloud Computing
Every time you stream a movie or TV show from Netflix, Hulu or Amazon, you’re using the cloud.
When personal computers first became available, all your software and data—the programs you used, the documents you created, every game, every photo, every piece of music or snippet of video—had to be stored on your computer’s hard drive. Then portable external hard drives became available, but all your software and data still lived somewhere in your office or home. Cloud computing changed all that. Now you can store data online—“in the cloud”—by keeping it in a place like Apple iCloud, Dropbox or Google Drive, where you can use a web browser like Chrome or Firefox to access it. You can run email in the cloud by using Gmail or Yahoo! Mail. Google Apps let you do word processing and spreadsheets through the cloud in a web browser, rather than by using software installed on your machine. And every time you stream a movie or TV show from Netflix, Hulu or Amazon, you’re using the cloud.

Putting It All Together

So how are wireless devices, sensors and the cloud combining to remake digital health? One example is the FitBit. The wrist-worn fitness tracker uses sensors to measure such health variables as steps walked, heart rate and calories burned. Then it uses a wireless connection to send that information to an app on a linked phone or computer, where you can log your workouts, track progress toward your goals and swap motivational messages with other users.
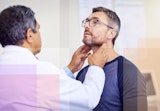
This merging of data will give providers a more holistic view of their patients’ health.
In addition, FitBit is now working with Google to develop a cloud-based data repository that will capture users’ FitBit data, keep it secure and make it available to health care providers, who will connect that information with their patients’ electronic medical records. This merging of data will give providers a more holistic view of their patients’ health, allowing them to provide more personalized care.
Like the FitBit, the Apple Watch boasts fitness-tracker functionality. Its sensors gather health data from the user’s body, and it uses a wireless connection to sync that data with a linked phone app or computer. Apple Watch users also have the option to upload their data through the cloud to IBM’s Watson Health secure cloud storage, where their health care providers will be able to access it.

The combination of these technologies has created an unbroken stream of health information that begins with the health status of your body and travels straight to the eyes of your doctor, who will use it to make treatment decisions. That’s digital health in its purest form.
Correct!
Incorrect
New Alternative to Colonoscopy is as Easy as Swallowing a PillExploring the Genome

Your genetic makeup is more than 99 percent identical to that of every other person on the planet.
Believe it or not, your genetic makeup is more than 99 percent identical to that of every other person on the planet. That fraction of a percent difference could explain why some people inherit rare diseases, such as cystic fibrosis, or develop more common conditions, including cancer and heart disease.
Health researchers are interested in genomics—the field of biology that focuses on the entirety of our genetic material—because it might help us eradicate disease at the most fundamental level. If we could find a genetic cause for a given disease, we might be able to develop a therapy that could repair the problem within the genome, where it first occurs.

And although most of your genetic makeup is shared in common with all of humanity, your specific genetic sequence is unique to you—which might make it possible to design treatments targeted to your genetic profile. Researchers are hard at work developing this type of medical intervention, known as precision medicine.
That genetic sequence is now stored in databases, available to anyone online.
The concept of precision medicine took a giant step closer to reality with the successful completion of the Human Genome Project in 2003, a 13-year international effort to identify the more than 3 billion letters in the human genome. That genetic sequence is now stored in databases, available to anyone online. Researchers around the world have dedicated their careers to exploiting the information contained in the human genome—genotyping viruses to discover the best treatments for them, identifying genetic mutations that cause cancers, creating targeted therapies and more.
Diagnosing, Predicting and Preventing Disease
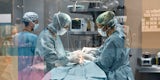
For instance, scientists have long known that cancerous tumors shed cells into bodily fluids. Now researchers are exploiting that fact to develop a “liquid biopsy” diagnostic test that detects the presence of cancer DNA in blood, saliva or urine, which may reduce or even replace the use of traditional tissue biopsies requiring needles or surgery.
Researchers are also working to discover the genetic causes of epilepsy. Scientists recently discovered 11 genes associated with epilepsy that were previously not known to be related to the condition. Now they can begin developing treatments that target those genes specifically, similar to the way they’re targeting the recently identified biomarkers for Parkinson’s disease.
Genetic testing can also be used to reveal increased risk for certain forms of cancer.
Genetic testing can also be used to reveal increased risk for certain forms of cancer. Mutations in genes BRCA1 and BRCA2, which produce tumor suppressor proteins, increase a person’s likelihood of developing breast or ovarian cancer. Seventy-two percent of women with BRCA1 and 69 percent with BRCA2 will develop breast cancer by age 80, while 44 percent with BRCA1 and 17 percent with BRCA2 will develop ovarian cancer. People who test positive for mutations in those genes face a major life decision: whether to have their breasts or ovaries removed in the hopes of avoiding cancer.

Today you can have your entire genome sequenced and sent to your smartphone in just a few weeks for less than $1,000.
Scientists still dream of a day when a person’s genome sequence becomes part of their medical chart, alongside blood pressure, weight and family history. We’re not there yet, but we’re getting close. Biotech companies have greatly advanced genome sequencing technology, and today you can have your entire genome sequenced and sent to your smartphone in just a few weeks for less than $1,000—down significantly from the $2.7 billion price tag for the first genome sequence.
Need Answers? Ask the AI
Humans are capable of astounding achievements. We built the pyramids, walked on the moon and invented the internet. But there are limits to our abilities; our brains can only work so fast, and we can only be in one place at a time.
Working in an AI Future
Learn More
To transcend those limits, many clinicians and medical companies are using artificial intelligence (AI) to perform tasks that were impossible until now. These computer systems, driven by state-of-the-art algorithms, can solve problems too complex for humans to crack or that would take us far longer to figure out. Health care providers can use AI to comb through reams of clinical text, patient data and medical imaging at unprecedented speeds. The goal: to find connections in disorganized data, spot patterns in the chaos, quickly make the right decisions and ultimately improve human health and well-being.
AI in Practice

AI may already be playing a role in your own medical care, as the U.S. Food and Drug Administration approves more and more AI algorithms for use in diagnosis and treatment.
For example, the clinical decision support tool Viz LVO uses AI to analyze CT scan images of the brain to check for indications that a patient has had a stroke and needs immediate medical attention. If the tool finds signs of a stroke, such as a blocked vessel, it notifies a neurovascular specialist who can give the patient a more intensive evaluation. Another program that analyzes medical imaging, OsteoDetect, uses an AI algorithm to check X-ray images for a common wrist fracture.
AI is also making an impact on oncology. A May 2018 study in the Annals of Oncology showed that an AI developed by Google outperformed a group of 58 experienced dermatologists in detecting melanoma and benign moles.
The use of AI in digital health applications isn’t limited to specialized medical hardware and software; consumers can get in on the act, too. The Apple Watch made headlines when the FDA gave its approval for the device to include an atrial fibrillation-detecting algorithm and an electrical heart sensor that enables the wearer to take an electrocardiogram. The algorithm detects irregular heart rates and alerts the user to any problems.
The Challenge and Potential of Big Data
To doctors and patients, the results of an electrocardiogram, biopsy or genetic test are information—potentially crucial information that just might make the difference between life and death. But if you’re a computer scientist or software engineer, you know that once a piece of health information enters a computerized system somewhere, it becomes data. And thanks in part to the recent explosive proliferation of all types of personalized data, we’re now wrestling with data sets that are so large and complex, a whole new field of statistical analysis—data analytics—has sprung up to address the challenge of what we now call big data.

In health care, data sources include electronic patient records, hospital morbidity and mortality rates, diagnostic test results, medical imaging, clinical trial research, insurance and pharmacy records, and wearable devices, among others. Researchers and clinicians want to parse and analyze this data to find hitherto undiscovered patterns that may facilitate scientific breakthroughs and enhance care. Insurers and health systems want to use it to reduce costs while improving outcomes. But there’s so much data in so many formats, spread across countless disconnected sources—with more being created all the time—that finding the proverbial needle in the haystack is starting to look easy.

Goal: Health Data on 1 Million Americans
The ultimate goal is precision medicine targeted to the individual.
To address the problem of data living in separate organizational silos, two universities and a medical center have formed the Pittsburgh Health Data Alliance, which will leverage their combined expertise in medical research, computer science and front-line health care to derive insights from the full range of health data available to them.
Along the same lines, the U.S. National Institutes of Health launched the All of Us program in an effort to make big data even bigger. All of Us aims to gather health data from at least 1 million people living in the United States. The project will aggregate all that data to learn how individual differences in lifestyle, environment and biology affect human health. Their aim is to develop precision medicine targeted to the individual.

Another NIH initiative, Big Data to Knowledge, has invested hundreds of millions of dollars to help biomedical researchers develop the computational and analytical tools they need to extract useful information from big data, including procedures for sharing data and keeping it secure.

For many of us, our most obvious contribution to big data comes from wearable fitness trackers, such as the Apple Watch. To make use of that data, Apple and IBM are partnering to create a big data platform focused on health information. When Apple Watch users opt to share health data with IBM’s Watson Health analytics service, the platform will feed the rich trove of users’ health data through the powerful algorithms of Watson’s AI in hopes that the supercomputer can identify patterns and trends that would lead to new health care discoveries.
Rise of the (Tiny) Machines

Tech-minded innovators are driving the astounding advances in digital health. Often, their big ideas come in surprisingly small packages.
In a scientific field called nanotechnology, scientists build micromachines using components so small they can be measured in nanometers (1 nanometer = one billionth of a meter). Thanks to nanotechnology developments, health care providers now have the tools to make even greater impacts in rural and impoverished areas.
For example, researchers armed with smartphones, iPod Touches and a specialized attachment for them traveled to three community health clinics in Rwanda, where they screened nearly 100 people for HIV and syphilis.
The phone attachment, which costs $34 to make, works by routing a finger-prick blood sample through a maze of tiny channels. It uses antibodies specially labeled with gold nanoparticles to reveal the presence of HIV and syphilis, providing results within 15 minutes. Researchers were able to scan 41 patients on a single iPod charge.
Their scan results were 96 percent as accurate in detecting infections as standard laboratory tests—at a fraction of the cost.
Their scan results were 96 percent as accurate in detecting infections as standard laboratory tests—at a fraction of the cost. Since the researchers published their findings in 2015, they have been working to provide the screening tool to the world’s most remote areas.
The attachment used in Rwanda is an example of one of the most promising areas of nanotechnology—the “lab on a chip.” These screening devices shrink all the components necessary to diagnose a wide variety of diseases, from the flu to cancer, down to the size of a single silicon chip that can extract a great deal of information from extremely small fluid samples.
Small Tech, Big Impact

Nanotech could play a role in revolutionizing the way people with diabetes manage their blood-sugar levels. In the United States alone, more than 30 million people live with diabetes. That’s roughly 9 percent of the population, according to the Centers for Disease Control and Prevention.
To meet that need, researchers at the University of North Carolina and NC State have created a “smart insulin patch.” It’s a square no larger than a penny, covered in 121 needles as small as eyelashes. Nano-sized bubbles containing insulin and glucose-sensing enzymes pack each microneedle, releasing their contents whenever blood-sugar levels get too high.
The patch can be customized to account for an individual’s weight and sensitivity to insulin. It might have the potential to replace painful insulin shots, at least for some patients. Researchers announced the innovation in 2015 and have been working ever since to translate it from animal models to humans.
Scientists are also developing light-activated nanoparticles that can deliver cancer drugs.
Scientists are also developing light-activated nanoparticles that can deliver cancer drugs. A study out of Washington University in St. Louis found that the technique worked in mice with metastatic breast cancer and multiple myeloma. Researchers packaged light-sensitive drugs into nanoparticles, used light from traditional cancer-imaging techniques to trigger the drugs and watched the drugs produce free radicals that killed the cancer cells.
Technological Innovation: The Key to Digital Health
As information technology continues to become faster, cheaper and more powerful, the same changes will transform digital health. The newest developments include a smartwatch that takes your blood pressure, an AI tool that predicts when diabetics will experience low glucose and a wrist-worn device that uses machine learning to detect when seniors are experiencing a health decline.
And that’s just the beginning. Health researchers and care providers will keep finding new ways to use technologies such as genomics, AI and nanotech to combat illness and improve the human condition.
Next Section
The Future of Digital Health
Chapter 04 of 07
Explore the future implications of current trends in digital health.